(RxWiki News) Pulmonary embolism is a condition that can strike suddenly, sometimes with deadly consequences. New research on treatments for the condition could lead to better outcomes and understanding of risk factors.
A recent review of studies found that thrombolytic therapy (dissolving of blood clots) for pulmonary embolism lowered the risk of death compared to anticoagulant therapy (prevention of blood clots).
The researchers also found that thrombolytic therapy carried an increased risk for major bleeding in comparison to anticoagulant therapy.
"Ask your doctor if you are at risk for pulmonary embolism."
The lead author of this review was Saurav Chatterjee, MD, from the Division of Cardiology at St. Luke’s-Roosevelt Hospital Center of the Mount Sinai Health System in New York, New York.
The review included 16 studies published between 1970 and 2014 that compared thrombolytic therapy to anticoagulant therapy for pulmonary embolism patients.
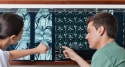
Pulmonary embolism is a condition in which one or more of the pulmonary arteries in the lungs become blocked, usually due to a blood clot. The pulmonary arteries carry deoxygenated blood from the heart to the lungs.
Thrombolytic therapy involves using medication to breakup blood clots, whereas anticoagulant therapy involves using medication to reduce the body’s ability to make clots in the first place.
Out of the 2,115 total study population, 10 percent of the participants had low-risk pulmonary embolism, 71 percent had intermediate-risk pulmonary embolism, 1 percent had high-risk pulmonary embolism, and 18 percent could not be classified.
Eight of the studies specified intermediate-risk pulmonary embolism patients. These studies included 1,775 patients.
The findings showed that thrombolytic therapy reduced the risk of death by 47 percent compared to anticoagulant therapy.
The patients who had thrombolytic therapy were 2.73 times more likely to have major bleeding, and 4.63 times more likely to have an intracranial hemorrhage, than those who received anticoagulant therapy.
The pulmonary embolism patients who were 65 years old and younger only had a 25 percent increased risk of major bleeding with thrombolytic therapy versus anticoagulant therapy.
The researchers discovered that thrombolytic therapy lowered the risk of recurrent pulmonary embolism by 60 percent compared to anticoagulant therapy.
When analysis was restricted to the eight studies that included intermediate-risk pulmonary embolism patients, thrombolytic therapy lowered the risk of death by 52 percent and increased the risk of major bleeding events by 3.19 times compared to anticoagulant therapy.
Dr. Chatterjee and team concluded that further research is needed to develop risk profiles for bleeding in specific groups of pulmonary embolism patients, especially elderly ones. More research is also needed to see if anticoagulant medication could be used in combination with thrombolytic therapy.
Lastly, these researchers noted that their findings might not apply to patients with low-risk pulmonary embolism.
The review was limited because definitions of major bleeding events were either not consistent across the studies or not provided at all. Also, the studies used various types and doses of thrombolytic medications, and the researchers did not have data on patient characteristics such as demographics or medical history.
This review was published on June 17 in JAMA.
The authors reported some financial disclosures. Michael R. Jaff, DO, reported having served as a consultant to AstraZeneca; having received support from EKOS Corporation, Embolitech, Boston Scientific and Cordis Corporation; and being a board member for VIVA Physicians, a 501(c)(3) not-for profit education and research organization.
Robert L. Wilensky, MD, reported being a member of the scientific advisory boards of Cardiostem, GenWay, Soteria and Vascular Magnetics and having equity interest in Johnson & Johnson.